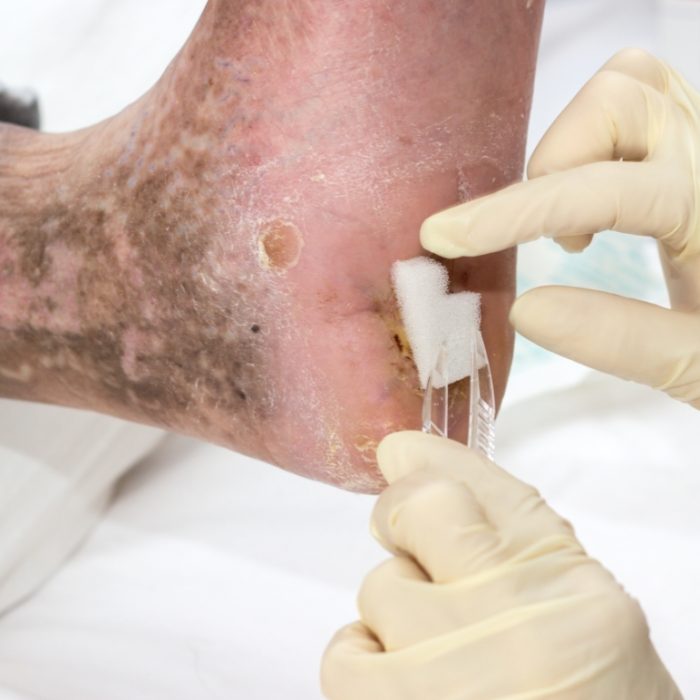
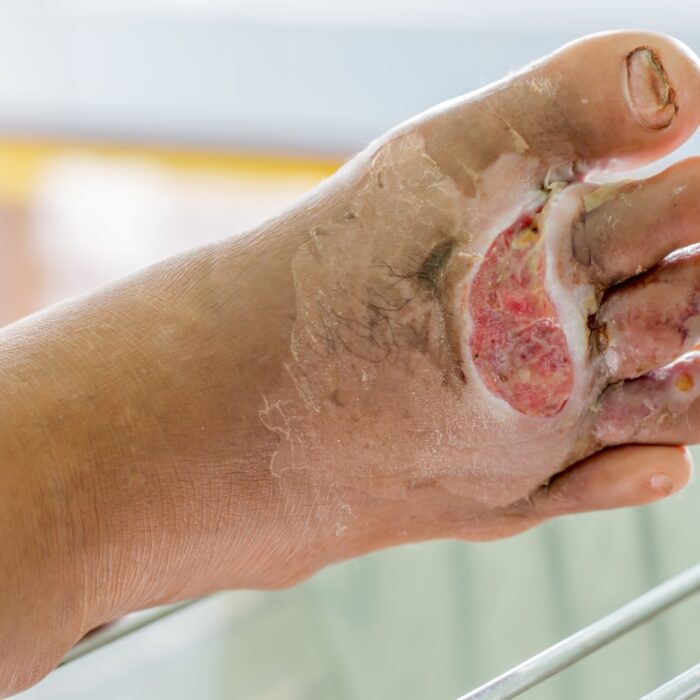
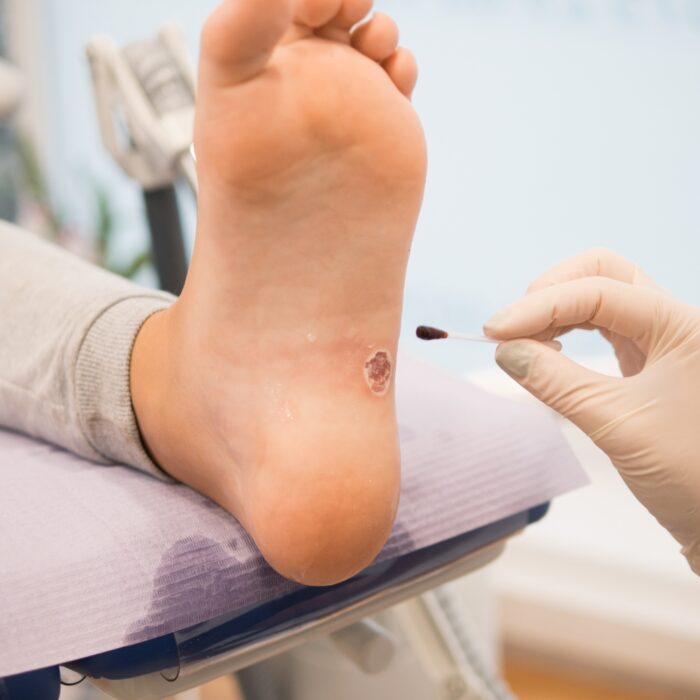
Wound Care Treatment & Healing
We utilize the most up-to-date approaches to wound healing
In 2018, Medicare reported that 8.2 million people had wounds, with or without infections, and that number is expected to increase exponentially each year.
Our teams approach to wound healing assesses wounds, makes a determination regarding treatment based upon advanced medical technology, and coordinates care of any other primary or underlying medical condition. These may be associated with complications from diabetes and other vascular disorders. We utilize the most up-to-date approaches to wound healing and we remain current on new scientific advances in wound care.
Peripheral artery disease (PAD) can be treated if diagnosed early and accordingly. There are warning signs and demographic factors that let you know if you may be at risk for PAD. Intermittent leg pain or cramps during routine movements, walking, or climbing up stairs could be common signs or symptoms of peripheral artery disease. Smoking, obesity and diabetes are all demographic factors that put you at greater risk of complications from PAD.
8 – 12 million Americans suffer from peripheral artery disease.
That’s more than all types of cancer combined. However, only around 40% exhibit symptoms and have been formally diagnosed with peripheral artery disease.
Studies show that, when treated early, up to 90% of peripheral artery disease related amputations can be avoided. Currently, as much as 25% of the diabetic population is at risk of losing some part of their leg or foot due to PAD.
Our expert team is available Mon-Fri 8am-5pm PST
Call today: (480) 788-5621
Schedule a Consultation
Please fill out the form below and a member of our team will promptly contact you!
Physician Evaluation
You will be evaluated thoroughly by a physician who will develop a comprehensive wound care protocol and detailed plan for your care. The physician is a surgeon who knows about wound healing, as opposed to emergency room doctors or internal medicine doctors who frequently see you at other wound care centers.
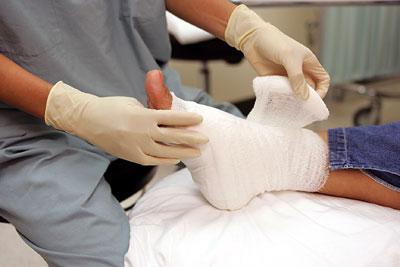
Debridement / Wound Wash and Care
Too much of fibrinous-exudate materials in the wound may impede and hinder wound healing. Our physician will debride and clean the wounds surgically in order to facilitate wound healing.
Vacuum-Controlled Assisted Closure (VAC) Therapy
is a system that uses controlled negative pressure (vacuum) to help promote wound healing. Clinical studies demonstrate that the VAC Therapy System also removes infectious materials and other fluids from the wound. The VAC Therapy System employs a computer-controlled therapy unit to maintain a constant negative pressure on the wound site.
Exercise Counseling
Exercise is important in preventing the development of pressure ulcers. Exercise prevents or decreases contractions of the muscles and joint deformities causes by stiffness and muscles weakness. Exercise also improves muscle tone and increases circulation. If you cannot move yourself, it is possible to imitate active exercise by asking someone to help you with exercises. These exercises are called range or motion exercises (R.O.M.) – meaning that you move each joint through its full motions. Remember while exercising to make movements as complete as possible in a slow, steady manner, but without causing pain. In the beginning, there may be slight discomfort, but this will improve as muscles and joints loosen. Use proper body mechanics while doing exercises. Do not bend or move with unnatural posture and use the larger muscles of the body to lift heavier items. A physical therapist, nurse or physician can help you determine specific exercises that are right for you. Generally speaking, each exercise should be repeated two to five times a session, once or twice a day (as advised), exercising both sides of the body.
Footwear Guidelines
Comfortable footwear is essential to the healthy progression of foot, ankle, and leg problems. Understanding how footwear can affect your health is an important step to recovery. We hope you consider the following footwear guidelines as a means to a better quality of life. The width and depth of shoes should allow for enough room to breathe without too much extra space. Footwear should not cause irritation, such as cramping or blisters. Your podiatrist may recommend custom footwear to provide proper sizing and support. Orthotics can be molded to your specific needs and provide an effective means of recovery. New shoes should be worn sparingly in order to adapt to a new feel. Similarly, it is important to change your shoes a few times a day, to reduce irritation and swelling. Wearing open-toed shoes should be discussed with your physician. Check your footwear for any foreign objects before putting them on your feet. Similar to footwear, socks should also fit properly and allow proper breathing. Choose a pair of socks with substantial padding to protect and support your feet. Never walk with bare feet!
Advanced Surgical Flap or Wound Surgery
In certain cases, advanced muscle flaps or wound surgeries may be required to facilitate quick healing of wounds. Our surgeons will coordinate surgical care if required.
Unna Boots
The best way to decrease swelling and promote healing of wounds in venous insufficiency or lymphedema patients. Our skilled staff will apply the boots, give you instructions, and stay in touch with you to maintain it well.
Nutrition Counseling
To heal pressure wounds and ulcers, it is important to eat foods that promote the healing process. These include lean proteins and multi vitamins including zinc and extra vitamin C, E, D, and A. The body uses extra calories when it is healing itself. Maintaining your weight is a good way to decide whether or not you are getting enough calories each day. Unless otherwise directed by a physician, the diet should be well balanced. A person with a wound should be weighed at least once a week. Our knowledgeable staff will assist you in obtaining optimum proteins, vitamins, and glucosamines to promote optimal healing.
We treat wounds of all types:
- Cellulitis
- Crushing Injury Wounds
- Dermatitis
- Pressure Ulcers
- Vascular Insufficiency
- Burns
- Complex Abdominal Wounds
- Diabetic Ulcers
- Abrasions
- Lacerations
- Lymphedema
- Mohs Surgery Non-healing wounds
- Ostomy and Fistula Care
- Radiation Wounds
- Skin Tears
- Surgical Incisions
- Peripheral vascular disease
- Collagen vascular disease